ISSN ONLINE(2319-8753)PRINT(2347-6710)
ISSN ONLINE(2319-8753)PRINT(2347-6710)
| Ashutosh D. Bagde 1 , Dr. S.B.Jaju 2 , Dr. P.G.Patil3 M.Tech scholar, G.H.Raisoni College Engineering, Nagpur 440016,Maharashtra, India1 Professor & Dean (R&D), G.H.Raisoni College Engineering, Nagpur 440016,Maharashtra, India2 Assistant Professor, Department of Prosthodontics, Government Dental College and Hospital, Nagpur 440003, Maharashtra, India 3 |
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Innovative Research in Science, Engineering and Technology
Various types of attachment techniques are available for overdenture implants. The design of removable overdenture for good retention & stability is difficult. This paper reviews various concepts involved in overdenture implant design and their comparison. It is seen that many treatment concepts involving mandibular overdenture are based on empirical experiences of individual. Clinicians often base their selection of implant location and attachment systems empirically on expected retentive quality. Various location methods are presented along with a comparison of Monovum i.e. single implant overdenture with other types of attachments.
Keywords |
| Overdenture, bar and clip attachment, ball attachment, single implant Overdenture |
INTRODUCTION |
| Tooth loss is a multifactorial and often a complex interaction of multiple comorbidities that, left unresolved, may progress to complete edentulism [1, 2]. Edentulism is defined as the state of being without natural teeth and represents a terminal process [3]. While the rate of edentulism has been decreasing throughout the past three decades, the subsequent increase in the world population has resulted in an increasing growth of total edentulous persons [3-4]. Between 1988 and 2002, the total percentage of edentulous individuals in the United States decreased from 10.5% to 8% [4, 5].During this same time period the total population increased from 245 million to 288 million individuals, representing a net decrease of over 2.6 million individuals when comparing edentulism rates across the entire population [5]. |
| These figures, however, do not accurately represent the true total number of edentulous dental arches because a substantially higher older population increase is expected to occur. This older cohort tends to have significantly higher levels of edentulism and the actual true number of edentulous arches is expected to rise from 57 million in 2000 to 61 million in 2020 [6]. As a result of the anticipated increase in edentulism, the demand for treatment will increase. Three main factors are involved in optimal denture treatment: retention, support, and stability [7, 8]. The overdenture has long been recognized as a method of maintaining alveolar ridge integrity and periodontal ligament mechanoreceptor, increasing denture stability, and, potentially, increasing retention. |
II. OVERDENTURE MATERIAL |
| The implant-retained mandibular overdenture generally consists of three main components: the implant, the abutment containing one half of the attachment system, and the overdenture prosthesis, which houses the other half of the attachment system [9]. The implants and abutments are made by metallic biomaterial while the overdenture is made by polymers. Various types of metallic biomaterials are available as listed in Table 1. The most commonly accepted biomaterial for implants and abutments are titanium and titanium alloy due to their good mechanical properties. [Table 1]. |
| Overdentures are made by using polymeric materials like acrylic resins. The various mechanical properties of different polymeric materials are shown in table 2. The treatment of the edentulous mandible with the 2 implant implant-retained is a well-accepted treatment option with long-term successful outcomes of prostheses and implants [10]. The use of stud-style attachments is considered a simplified and cost-effective treatment as compared to bar and clip type implant overdentures. The prosthetic and attachment system factors involved with treatment planning successful mandibular implant overdentures have been the subject of extensive investigations [11-12]. Included in this discussion is the anchorage design and space requirements, number of implants required, effect upon alveolar bone and anatomical factors, cost & maintenance, effects of antagonistic arch, stress distribution, and patient satisfaction. Missing from these discussions, however, is an analysis of implant location and distribution upon the aforementioned prosthetic factors |
 |
II. TESTING FOR RENTENTION |
| Two types of attachment for mandibular overdenture are available. First is stud type and another is bar & clip type. In stud 4 type of commercial stud are available as shown in fig.1. To determine the optimum type of stud various experiments was carried out for finding highest sustainable dislodgment force |
 |
| Wahab and Sadig designed several models for testing magnetic retention of overdentures including one two-implant model, two four implant models, and one six implant model [14]. The authors were able to determine that retention and stability of overdentures could be improved by altering implant location and distribution. Fatalla et al investigated distribution of implants according to two main designs: triangular versus quadrangular support [15]. The authors determined that after cyclic loading and wear analysis that wide, even distribution of attachments provided the highest level of retention and stability. In consideration of the currently available studies, limited information exists regarding implant position, distribution, and number and the effect upon the retention and stability of Mandibular implant overdentures. |
| The purpose of our investigation is to find out the effect of implant location, distribution and number upon the magnitude of force required to dislodge implant overdenture prostheses by using modern CAD/CAM technique for ball type attachment and bar & clip type attachment. |
| A. Testing Parameters for ball type attachment |
| Scherer has performed the test by dividing 2 patrix portions of the attachment system were placed into areas designed as group numbers that approximate natural tooth positions: group 1 (#23,26), group 2 (#22,27), group 3 (#21,28), group 4 (#20,29), group 5 (#18,31). (Fig 5) Matrix housing portions of the attachment system were attached to the prosthesis following manufacturer guidelines with a bis-acryl material (ERA, PickUp, Sterngold, and Attleboro, MA) [16]. |
 |
| Scherer has evaluated result as follow: |
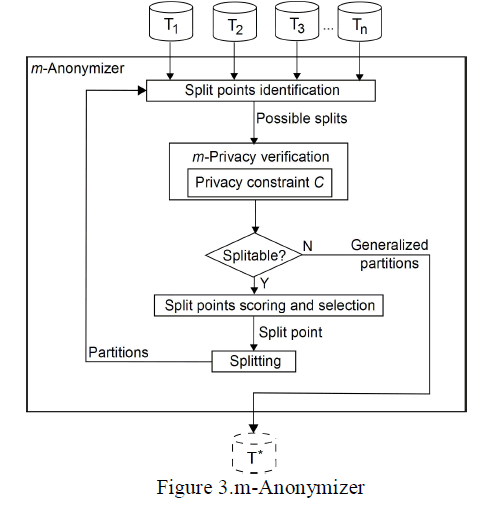
| a) In the vertically directed test, peak load means ranged from 7.43 N to 37.17 N. Fig.2 |
| b) Ball attachments had the highest mean retentive value and ERA orange had the lowest mean retentive value (Ball clear > Locator pink > O-Ring standard > ERA orange). Fig. 3 |
| c) In the obliquely directed test, peak load means ranged from 4.84 N to 20.23 N. Fig.3 |
| d) Ball attachments had the highest mean retentive value and ERA had the lowest. mean retentive value (Ball clear > Locator pink > O-Ring standard > ERA orange). Fig 4 |
 |
 |
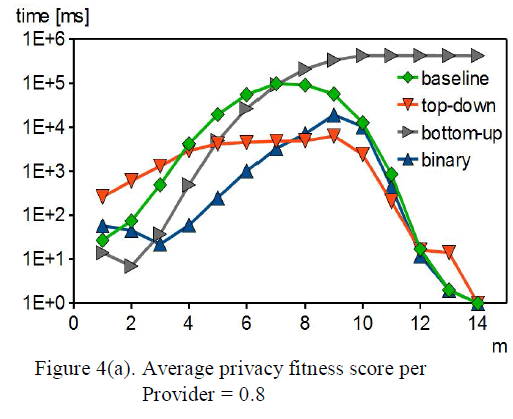
| e) In the antero-posteriorly directed test, peak load means ranged from 5.92 N to 31.28 N. Fig. |
| f) Ball attachments had the highest mean retentive value and ERA had the lowest mean retentive value (Ball clear > Locator pink > O-Ring standard > ERA orange). Fig 5 |
 |
| This all results help us to concentrate our study towards only ball attachment out of available different four attachments shown in fig 1. |
| B. FEM TESTING FOR BAR AND CLIP ATTACHMENT |
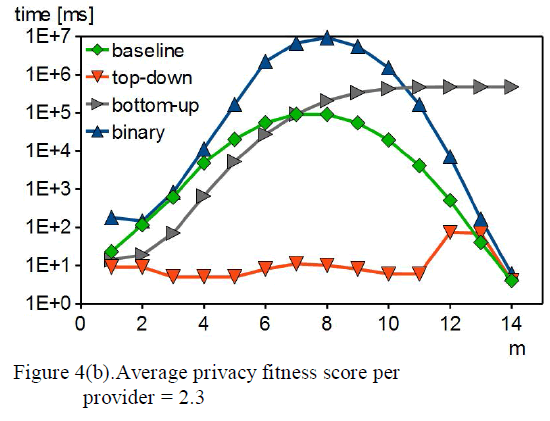
| Prakash et al perform the comparative study for various types of bar and clip attachment with the use of FEA. Three different models with three different configurations are prepared. Model 1single bar connecting two implants. Model2 had three bar connecting four implant. Model3 had two bar connecting medial & distal implant on the side only. The model is loaded under static condition with 100N load distributed at approximate position of clip. The mandible boundary conditions were modeled considering real geometry of its muscle supporting system. [16]The authors have found that stress at bar & bone implant interface is minimum in four implant bar system than in two bar system. We perform the evaluation of this result for the clinical advantages along with comparison with the ball attachment. |
 |
IV. THE MONUVUM |
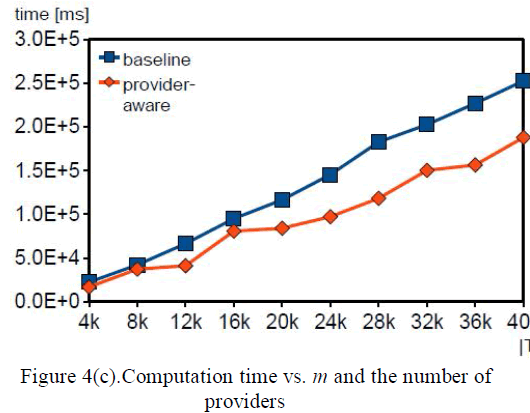
| One disadvantage of bar constructions is limited hygiene and the possible development of mucosal hyperplasia [17]. Beside that Single-implant–supported overdentures may be appropriate for the treatment of edentulism in geriatric patient groups because of demised functional demands and the realization that implant/patient life expectancy is limited [18]. As a result we are going for FEM analysis single tooth implant commonly known as Monovum. |
 |
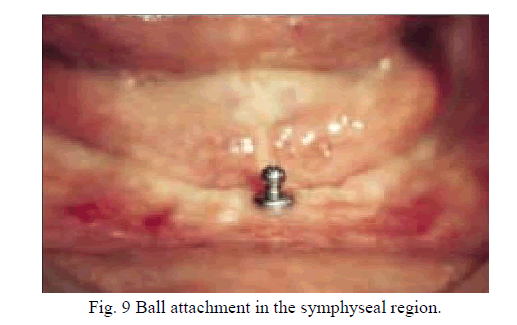 |
V. DISCUSSION |
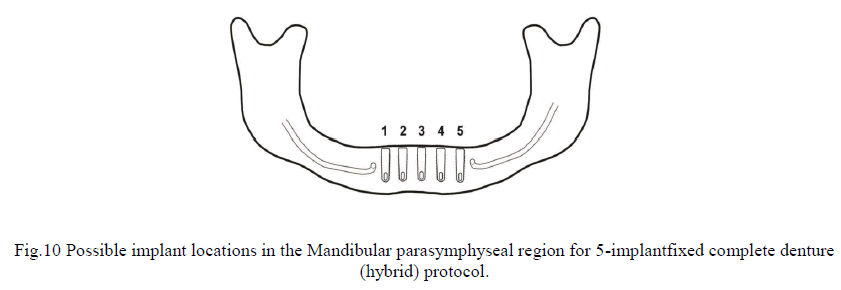
| Treatment evaluation of patient’s who present with edentulous mandibles involves teamwork between surgical and prosthetic approaches. Patients may be presented with several different options for implant prosthetic reconstruction that include: fixed metal-ceramic restorations, fixed complete denture restorations (hybrid), implant-supported removable overdentures, and implant-retained removable overdentures [19]. Surgical treatment has been well established for implant placement in the parasymphyseal region of the edentulous mandible for fixed and removable restorations [20-21]. Following the established 5-implant hybrid technique, figure 10 shows 5 possible locations for implant placement. Implants #1, 5 are placed first based upon location and a recognized 3-5-mm safety zone anterior to the mental foramen. [22-23]. After locating the Mandibular parasymphseal midline, implant #3 is placed slightly to the right or left of the suture line. Marking the midline between #1/3 and #3/5, the surgeon places implants #2/4 last. Based upon historical Overdenture therapy, restorative clinicians typically request the surgeons to place implants at the Mandibular canine locations or #2/4 sites. If the implants are placed too far medially or distally in relation to proposed additional implant sites, encroachment of implants may occur which may lead to complications [24]. From the results of this study, one can conclude that retention and stability of an implant-retained Overdenture may be similar between implants at the Mandibular canine location (#2/4) as compared to implants at the Mandibular 1st premolar location (#1/5). |
 |
| Mandibular overdentures, when in place in the oral environment, move in complex ways. Movement of overdentures typically occurs in six directions: occlusal, gingival, mesial, distal, facial, and lingual. While true unidirectional dislodging forcesrarely occur in clinical scenarios, directional pull-testing is an effective way of measuring retention and stability of a prosthesis during in vitro laboratory evaluation [25-26]. |
VI. CONCLUSION |
| It is evident that many treatment concepts involving Mandibular overdentures are based on empirical experiences of individuals [27-28]. Implant location and attachment system empirically on expected retentive qualities. Evaluating these factors the results allow the clinician to formulate a comparison of implant location to retention and stability of an implant-retained Overdenture prosthesis |
| The results of this review investigation indicate that implant location, distribution, and number affect in vitro retention and stability of an implant overdenture. The study reveals that vertical retention increases with increasing implant number and distribution. In the vertical pull tests, the single implant reported the lowest mean retentive values and steadily increased as implant number was increased. The largest increase occurred when comparing single implants versus two; retention doubled for most systems. The type of attachment affects the effect of vertically applied forces. Horizontal displacement forces increase with increasing implant number and distribution except in the two implant model. In the oblique pull tests, the results varied tremendously depending on the type of attachment utilized. The results of this study indicate that single ball attachments, and 2, 3, or 4 widely spaced implants may be an effective therapeutic protocol for use in implant-retained Overdenture therapy. A single implant and ball attachment may provide adequate retention [16]. Attachment type affects retention and stability differently by location. Ball attachments reported the highest levels of retention and stability. |
| It has been found that overdenture implants are studied for retention and stability are concluded by direct experiment or clinical case study. While the effects of biomechanics on overdenture especially in stud type are untouched. This area should be study to use modern engineering technique like FEM in dental science for obtaining the optimum implant location with proper analysis. |
ACKNOWLEDGEMENT |
| Dr. Harish Rathi, Advance Dental Hospital, Sadar, Nagpur. Dr. Nakul Rathi BDS, MS The Ohio State University. |
References |
|