ISSN ONLINE(2319-8753)PRINT(2347-6710)
ISSN ONLINE(2319-8753)PRINT(2347-6710)
G Durgadevi1, P Jamuna2, J Janet Priskilla 2, M Princy2
|
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Innovative Research in Science, Engineering and Technology
Pressure ulcers are wounds caused to skin and tissue lying beneath because of persistent pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such us the heels, ankles, hips and tailbone. People mostly affected by bedsores are those with a poor medical condition that has removed their ability to adjust positions, necessitate them to use a wheelchair or confines them to a bed for a long time. Bedsores can easily develop and are often difficult to treat. Pressure ulcer, also known as pressure sores or bed sores is found to prevail in 10% of hospitalized patients as per the statistical report provided by the National Center of Health Statistics (NCHS) in the year 2009. Yet another report provided by the Agency for Health care Research and Quality (AHRQ) divulges a fear-provoking reality that 1-25 percent of admitted patients with this particular setback, terminated in death. This poses a serious threat of 2.5 million patients being affected per year.Pressure ulcers cost several billion dollars per year in the US. Cost of individual patient care ranges from $20,900 to 151,700 per pressure ulcer. Medicare estimated in 2007 that each pressure ulcer added $43,180 in costs to a hospital stay. Pressure ulcers may be associated with severe pain. About 60,000 patients die as a direct result of a pressure ulcer each year. More than 17,000 lawsuits are related to pressure ulcers annually. It is the second most common claim after wrongful death and greater than falls or emotional distress.
NEED FOR THIS WORK |
| As per the report provided by the Pennsylvania Patient Safety Reporting System (PA-PSRS) progression of pressure ulcers takes place in four stages. Which can be noted from table 1. |
 |
| The initial stages of these ulcers are somewhat curable whereas at the final stages this becomes impossible to treat. Therefore the only method to prevent this problem is to monitor the patients’ body pressure in the early stage .Although some of the pressure relieving systems does exist but they are either uneconomical or painful. In countries like India patient doctor relation is unsatisfactory. Therefore there is a need for an automated pressure relieving system. |
FACTORS CAUSING PRESSURE ULCERS AND SYMPTOMS |
| The factors causing pressure ulcers are shown below in figure 1. |
 |
| Bedsores can be grouped into four stages based on the level of complexity. A professional organization called National Pressure Ulcer Advisory Panel that endorses the prevention |
 |
| and treatment of pressure ulcers and defines each stage. The four stages of pressure ulcer is shown in figure2. |
| In the beginning stage of a pressure sore the skin is remains intact whereas the skin appears red on people with lighter skin color. In case of people darker skin, the skin may show discoloration. The site affected by pressure ulcer may be tender, painful, firm, soft, warm or cool compared with the surrounding skin. At the second stage, the external layer of skin (epidermis) and the layer beneath it (dermis) is damaged or lost and the skin deepens and becomes pinkish red finally forms into a fluid-filled blister or a ruptured blister. When the third stage commences, the ulcer becomes a deep wound and the skin breaks up and exposes some fat. The tissues beneath the ulcer tissue become dead and the damage may spread into the healthy layers of the skin. At stage four ulcers shows large-scale loss of tissue and the muscle is exposed because of the wound, bone or tendons .The bottom of the wound likely contains dead tissue that's yellowish or dark and crusty. The damage often extends beyond the primary wound below layers of healthy skin. A pressure ulcer is considered unstageable if its surface is covered with yellow, brown, black or dead tissue. It’s not possible to see how deep the wound is. |
EFFECTS OF PRESSURE ULCERS |
| Pressure ulcers cause enormous pain and discomfort to the patients. Physically the pain experienced is unbearable. This is the physically affected parameter but there are psychological parameters because the patients don’t get adequate care from their care givers in most developing countries. This is a very serious problem which at most times not taken much care but if not identified and treated this can ultimately lead to death of the individual. |
CAUSES OF PRESSURE ULCERS |
| The major causes of pressure ulcers include excessive shear force on a particular region or the compression of tissues and ultimately destruction of muscle cells. In most of the cases, this compression is caused when the bone rubs against a surface, such as when a person remains in a single position for a long period of time. After a persistent period of time with limited blood flow to tissues and leads to tissue death if left untreated. Shearing is a force exerted when a person's skin stays in one place and cause the pinching off of the blood vessels which may lead to tissue death. Friction plays an important role in causing pressure ulcers. Temperature is also one of the important factors causing pressure ulcer. The cutaneous metabolic demand rises by 13% for every 1 °C rise in cutaneous temperature. When supply cannot meet demand, then pressure ulcer occurs. At present two major theories about the development of pressure ulcers coexist. The first and most accepted is the deep tissue injury theory which claims that the ulcers begin at the deepest level, around the bone, and move outward until they reach the epidermis. The second, less popular theory is the top-to-bottom model which says that skin first begins to deteriorate at the surface and then proceeds inward. |
RISK FACTORS |
| Most people are at risk of developing pressure sores if they have inconvenience in moving and are not able to easily change position while seated or in bed. Immobility may result due to certain factors such as poor health or weakness, paralysis and injury or illness that requires bed rest or wheelchair .Theother factors that aggravate the risk of pressure sores include age, lack of sensory perception, weight loss, poor nutrition and hydration, excess moisture or dryness, bowel incontinence, medical conditions affecting blood flow, smoking, limited alertness and muscle spasms. Usually the skin of older community of people is more prone to damages. Also the rate of growth of skin cells is much slower when compared to younger people. These feature makes skin vulnerable to damage. Any damage to the spinal cord, nervous disorders and other conditions can result in a loss of sensation. If the senses are lost then the person won’t be aware of bedsores or the necessity and importance to change position. Weight loss is common during prolonged illnesses, and muscle atrophy and wasting are common in people with paralysis. |
| The loss of fat and muscle results in less cushioning between bones and a bed or a wheelchair. People need enough fluids, calories, protein, vitamins and minerals in their daily diet to maintain healthy skin and prevent the breakdown of tissues. Skin that is moist from sweat or lack of bladder control is more likely to be injured and increases the friction between the skin and clothing or bedding. Very dry skin increases friction as well. Bacteria from fecal matter can cause serious local infections and lead to life-threatening infections affecting the whole body. Health problems that can affect blood flow, such as diabetes and vascular disease, increase the risk of tissue damage. Smoking reduces blood flow and limits the amount of oxygen in the blood. |
| Smokers tend to develop more-severe wounds, and their wounds heal more slowly. People whose mental awareness is lessened by disease, trauma or medications may be unable to take the actions needed to prevent or care for pressure sores. People who have frequent muscle spasms or other involuntary muscle movement may be at increased risk of pressure sores from frequent friction and shearing. |
AFFECTED AREAS |
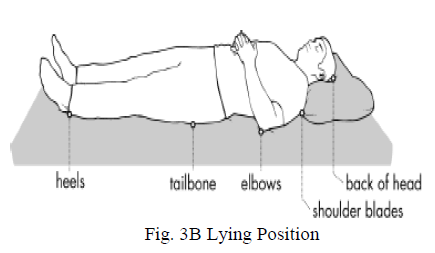
| Areas where bones are close to the surface and areas that are under the most pressure are at greatest risk for developing pressure sores. The areas affected changes depending upon the posture of the patient. The most important pressure points include back of the head, shoulder blades, elbows, tail bone and heels. The figure 3A, 3B and 3C shows the different affected areas. |
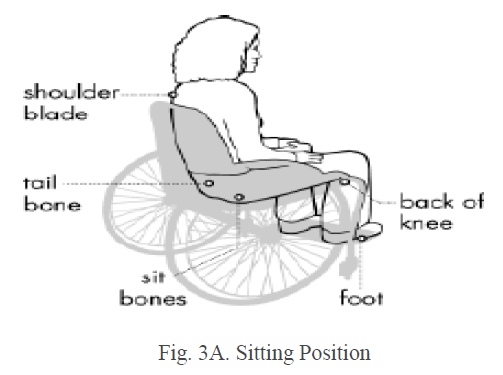 |
| In order to keep the body parts free from pressure they can be padded with pillows or foam. One can place a pillow between the knees while sleeping on the side to prevent skin-to-skin contact and increase air circulation between the legs. |
 |
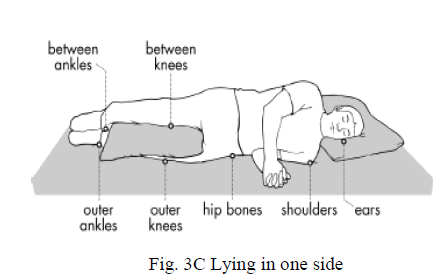 |
| Pressure sores are usually caused by unrelieved pressure on the skin. They often form on skin that covers bony areas. The most common sites are the back of the head and ears, the shoulders, the elbows, the lower back and buttocks, the hips, the inner knees, and the heels. Pressure sores may also form in places of the skin folding over itself. |
AVAILABLE TECHNOLOGIES |
| At present there are only a few technologies available in order to avoid pressure ulcers. One such solution is the repositioning and using support surfaces. If a person has a pressure sore, he needs to be repositioned regularly and placed in correct positions. In case he uses a wheelchair, one has to try shifting the weight every 15 minutes or so. Therefore the person needs help to be repositioned every hour. If he is confined to a bed, the position has to be changed for every two hours. If he has enough upper body strength, one must try repositioning himself using a device such as a trapeze bar. Caregivers can use bed linens to help lift and reposition the patient. This can reduce friction and shearing. A mattress, bed and special cushions can be used that can help the patient to lie in an appropriate position, relieve pressure on any sores and protect vulnerable skin. If confined to a wheelchair, a cushion is preferable. Styles include foam, air filled and water filled. Out of this any one which suits the patients’ body condition, body type and mobility can be chosen. |
CONCLUSION |
| In the systems analyzed so far one could find only a pressure monitoring system. Even if pressure relief procedures exist but it is not affordable to common people, like the air mattresses used in foreign countries. Therefore it is very important to design a pressure monitoring system along with a pressure relief which would provide an independent solution for the patients. |
References |
|