ISSN ONLINE(2319-8753)PRINT(2347-6710)
ISSN ONLINE(2319-8753)PRINT(2347-6710)
Taher Abdel-Aziz1,Naglaa Azab2, Mossad Odah 3, I.M. El-deen4
|
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Innovative Research in Science, Engineering and Technology
In this study we tested some factors associated with the prediction of hyperbilirubinemia of the newborn as cord, first day bilirubin blood levels, ABO, Rh incompatibility and use of oxytocin. This was conducted on 384 healthy term newborns, they were followed up for first 3 days of life. We analyzed bilirubin levels in cord blood and serum of the baby in first day [1]. Any baby had total serum bilirubin (TSB) more than 17mg/dL considered as having significant hyperbilirubinemia.16.1% of included newborns developed significant hyperbiliruinemia. ROC curve analysis demonstrates that the cord blood bilirubin cut off point 2.38mg/dL, and first day bilirubin cut off point 5mg/dL .There was statistically significant relation between cord bilirubin level, first day bilirubin level and subsequent hyperbilirubinemia (P <0.01).We conclude that newborns having umbilical cord blood bilirubin level >2.38 mg/dL or first day (TSB)>5 mg/ dL should be followed up in the first 3 days of life.
Keywords |
| hyperbilirubinemia, hospitalization, cord bilirubin, TSB. |
INTRODUCTION |
| Jaundice is the visible manifestation in skin and sclera of elevated serum concentration of bilirubin [1].Jaundice is observed in approximately 60% of term and 80 % of preterm neonate during the first week of life[2]. Neonatal jaundice may not appear until serum bilirubin exceeds 5 to 7 mg/dL. Any serum total bilirubin (STB) elevation exceeding 17 mg/dL (291μmol/l) is considered pathologic and warrants investigations for a cause and possible therapeutic intervention[1].Neonatal hyperbilirubinaemia is the most common reason of readmission after early hospital discharge. Concerns regarding jaundice have increased after reports of bilirubin induced brain damage occurring in healthy term infants even without haemolysis[3]. Recently, concern has been expressed that the increase in early hospital discharges, coupled with arise in breast feeding rates, has led to a rise in the rate of kernicterus resulting from “unattended to” hyperbilirubinemia [4].The American academy of pediatrics (AAP) recommends that newborns discharged within 48 hours should have a follow up visit after 2-3 days to detect significant jaundice and other problems [2].Because of medical and socialreasons and sometime economic constraints, early discharge of healthy term newborn infants become a common practice, so reliable strategies can reduce hospital stay for normal babies and identify significant hyperbilirubinemia that may be happened in the future. |
II-METHODS |
| This prospective study was performed at Benha university hospital over a period of 8 months. Threehundred eighty four healthy full-term newborns born at this hospital during this period were included in this study, 181 males and 203 females. Cord bilirubin estimation was performed at birth and babies total serum bilirubin was estimated at 1st 24 hours and followed up during first 3 days of life [1]. Selection and Description of Participants |
| In all cases maternal and neonatal data were collected which includes route of delivery,gender of the baby, birth weight, feeding pattern, Apgar scores, and whether there were any siblings with neonatal jaundice, oxytocin used or not during delivery ,blood group of mothers and infants. Consent was obtained verbally from all parents of the newborns included in the study. We ensured that subjects included in the study should be of gestational age (38 to 42weeks), Apgar score equal to or more than 7 at 5th minute of delivery and birth weight equal to or more than 2500 grams. The following babies were excluded before beginning of the study: any born with any critical illness as sepsis, major congenital Malformations or birth trauma. |
III-STATISTICAL ANALYSIS |
| Descriptive data are presented as mean and standard deviation.. Relationship between measurements was assessed by Pearson’s correlation co-efficient. ROC analysis was used to demonstrate sensitivity, specificity, negative and positive predictive values of cut- points of cord bilirubin and first day bilirubin. For all the tests, a p value of 0.05 or less was considered for statistical significance. |
IV-RESULTS |
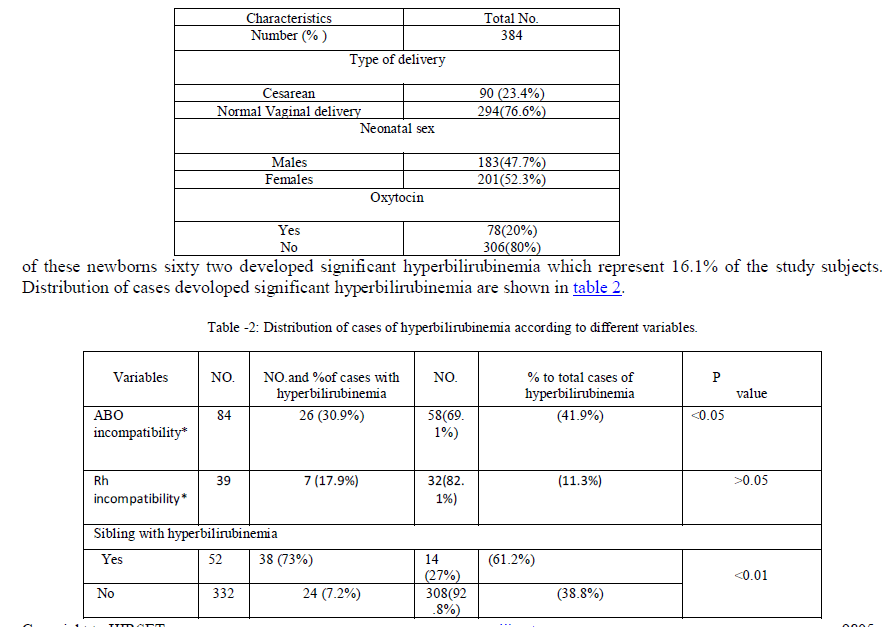
| Three hundred eighty four healthy full-term newborns were the subjects of this study. Characteristics of the included subjects are shown in table 1.s |
| Table 1: Characteristics of infants and their mothers. |
 |
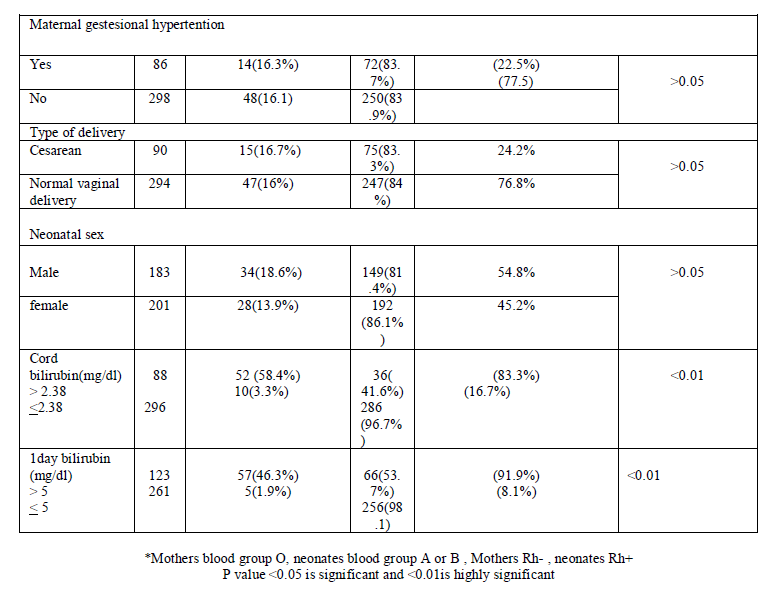 |
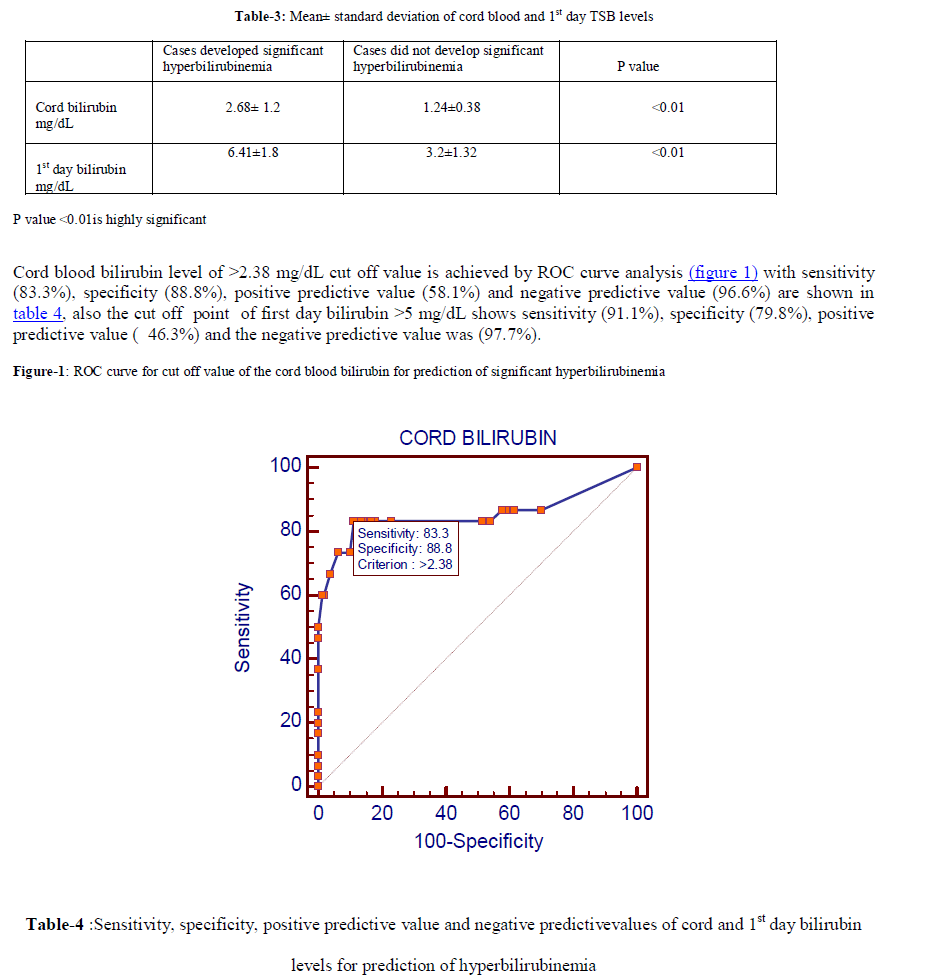
| It shows the significant relation between siblings with jaundice, ABO incompatibility, use of oxytocin, cord bilirubin level, first day bilirubin level and development of hyperbilirubinemia (P<0.05).There were no significant differences between the cases who did and who did not develop significant hyperbilirubinemia with respect to various factors that may be associated with the risk of hyperbilirubinemia, such as, type of delivery, Rh incompatibility, maternal gestational hypertention and sex of the baby (P value > 0.05). The percentage of ABO incompatibility was 21.8% and 30.9% of these infants had hyperbilirubinemia. The percentage of Rh incompatibility was 9.6% and 17.9% of these infants had hyperbilirubinemia. Hyperbilirubinemia was observed in 37.2% of infants whom mothers had received oxytocin and 10.8% of infants whom mothers had not receivedoxytocin. 13.5% of study subjects had sibling with pathological jaundice and 73% of them had significant hyperbilirubinemia, table 2 also shows that hyperbilirubinemia developed in 3.3% of newborns with cord bilirubin less than 2.38mg/dl and in58.1%of newborns with cord bilirubin >2.38mg/dL, hyperbilirubinemia developed in 1.9% of newborns with first day bilirubin less than 5mg/dl and in 46.3%of newborns with first day bilirubin >5 mg/dL. Table 3 shows the mean and standard deviation of cord blood bilirubin and 1st day TSB in cases did and did not develop significant hyperbilirubinemia. Cases developed significant hyperbilirubinemia showed cord bilirubin level 2.68± 1.2 mg/dL and 1st day bilirubin level 6.41±1.8 mg/dL while cases did not develop significant hyperbilirubinemia showed cord bilirubin level 1.24±0.38 mg/dL and 1st day serum bilirubin level 3.2±1.32 mg/dL . There is significant difference between cases developed and cases did not develop significant hyperbilirubinemia regarding to cord blood bilirubin level and 1st day serum bilirubin levels (P<0.05). |
 |
 |
V-DISCUSSION |
| Hyperbilirubinemia is one of the most common problems encountered in term newborns.There is concern about an increasing incidence of hyperbilirubinemia and possibility of kernicterus in healthy term neonates, hyperbilirubinemia is one of the most common causes of readmission of newborns. the need for prediction of healthy neonates at risk for hyperbilirubinemia limits stay in hospital and allows simple bilirubin reducing methods to be implemented before bilirubin level reaches critical levels .In recent years, lot of efforts have gone in to predict babies likely to develop neonatal hyperbilirubinemia. Reliable predictors can reduce hospital stay for normal babies resulting in discharge and identifying at risk or high risk neonates likely to develop pathological jaundice. We have assessed the ability of cord blood and first day bilirubin levels in predicting infant at high risk for post natal hyperbilirubinemia. The incidence of significant hyperbilirubinemia depend on regional variations, ethnic composition of the population, laboratory variability of the measurement of bilirubin and the incidence of breast feeding [5]. In our study the incidence of pathological hyperbilirubinemia was 62 (16.1%). Our study subjects showed no significant relation between the sex or the mode of delivery of the infant and the development of significant hyperbilirubinemia (p > 0.05), this was in agree with most of the studies asTaskande et al[6]and Sun et al [7] and not go with other studies regarding to the sex as study ofGatea [2], Maisels and Kring [8]. Our study also shows no significant relation between serum bilirubin level and maternal gestational hypertention, this coincide with the other studies such as the study ofTaskande et al[6], Awasthi and Rehman[9]. Rh incompatibility subjects showed higher susceptibility to develop hyperbilirubinemia but still no significant relation seen, this goes with the study of Gatea [2]. In our study there was significant association between the induction of labour with oxytocin and the neonatal hyperbilirubinemia (P<0.05). Our study is in correlation of the study ofRostami and Mehrabi[10], Oral et al [11] and not in correlation with study of Taskande et al[6] and Gatea [2]. We observe high significant association between the presence of sibling with hyperbilirubinemia and the development of significant hyperbilirubinemia (P<0.01).this is consistent with the other studies e.g. Lavanya et al[12]. High significant association was observed between the ABO incompatibility and the development of hyperbilirubinemia. The number of ABO incompatibility in our study was 84 and 30.9%of them which represent 40.9% of the total hyperbilirubinemic infant (P<0.01) developed significant hyperbilirubinemia, this is consistent with results from other studies e.g . Knüpfer et al[13]. |
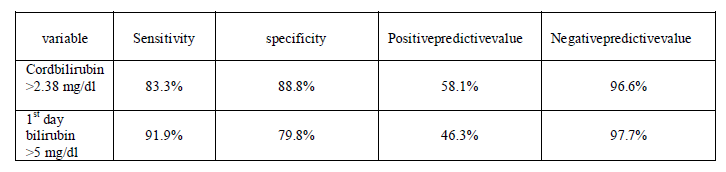
| The probability that neonates with cord bilirubin >2.38mg/dl would later become hyperbilirubinemic (positive predictive values) was 58.1%. The negative predictive value, the probability of non hyperbilirubinemia given a cord bilirubin lower or equal to 2.38mg/dL was 96.6%. If a child becomes hyperbilirubinemic, the probability that the cord bilirubin was higher than 2.38mg/dL was 83.3% (Sensitivity). The probability that a cord bilirubin level lower or equal to 2.38 mg/dL in neonates without hyperbilirubinemia was 88.8% (Specificity). However, the cord bilirubin level of less than 2.38 mg/dL has not completely exclude the development of significant hyperbilirubinemia, 3.3% of the newborns with cord bilirubin levels of less than 2.38mg/dL have developed hyperbilirubinemia, 96.6% negative predictive value in our study suggests that measurement of cord serum bilirubin can help in identify those newborns who are unlikely to require further evaluation and intervention. Several studies published the usefulness of cord bilirubin level in prediction of development of neonatal hyperbilirubinemia , for example in the study ofNaharet al[3], the cut off value was 2.5 mg/ dL, while study ofTaskande et al[6] proposed 2 mg/dL as cord bilirubin cut off value of the newborns. In our study, on ROC curve analysis, critical first day bilirubin level with high sensitivity and high specificity more than 5 mg/dL was selected, it shows sensitivity 91.9% , specificity 79.8%, positive predictive value 46.3% and negative predictive value 97.7%. Only 1.9% of the newborns with 1st day bilirubin levels of less than 5 mg/dL have developed hyperbilirubinemia, 97.7 % negative predictive value in our study suggests that measurement of 1st day serum bilirubin can help more efficiently in identifying those newborns who are unlikely to require further evaluation and intervention. Other study also suggested the 1st day bilirubin level as a predictor for significant hyper bilirubinemia [14], he stated 6.4 mg/dL as a cut off value. |
VI-CONCLUSION |
| Cord blood bilirubin and TSB values can help in identification of infants at low or high risk for hyperbilirubinemia and minimize an unnecessary prolongation of hospitalization. Cord bilirubin level of >2.38 mg/dL in healthy term newborns can predict development of significant hyperbilirubinemia. 1st postnatal day bilirubin estimation with bilirubin level more than 5 mg/dL can also be used and more efficiently as an early predictor of neonatal hyperbilirubinemia. |
References |
|