ISSN ONLINE(2319-8753)PRINT(2347-6710)
ISSN ONLINE(2319-8753)PRINT(2347-6710)
Parva Jani1*, Gunjan Patel1,Khushboo Patel1,Shivani Patel1, Hitesh Jain1, Prasanna Pradhan1
|
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Innovative Research in Science, Engineering and Technology
Diabetes is a disease in which levels of blood glucose, also called blood sugar, are above normal. Normally, after a meal, the body breaks food down into glucose, which the blood carries to cells throughout the body. Cells use insulin, a hormone made in the pancreas, to help them convert blood glucose into energy. People develop diabetes because the pancreas does not make enough insulin or because the cells in the muscles, liver, and fat do not use insulin properly, or both. As a result, the amount of glucose in the blood increases while the cells are starved of energy. Over the years, high blood glucose, also called hyperglycaemia, damages nerves and blood vessels, which can lead to complications such as heart disease, stroke, kidney disease, blindness, nerve problems, gum infections, and amputation. Diabetic patients are generally advised to check their blood glucose every day. Since the all current existing conventional methods of home blood glucose tests are painful, intimidating, laborious, and expensive, since they require obtaining a blood sample by pricking a fingertip with a needle or lancet. Thus it is necessary to develop a non-invasive blood glucose measurement method which could provide fast, painless, and convenient glucose monitoring to diabetic patients. The ophthalmic glucose monitoring system is a non-invasive method of determination of blood glucose and consists of wearable contact lenses which are equipped with sensors which detect glucose level in the lachrymal fluid which can be correlated with blood glucose level.
Keywords |
| Diabetes, Blood glucose, Non-invasive, Contact lenses, lachrymal fluid |
INTRODUCTION |
| The blood glucose can be measured by the following conventional methods |
| 1. From urine analysis |
| 2. From blood analysis |
From urine analysis |
| Self-testing of urine using Benedict’s copper reagent required heat for colour development, which presented practical difficulties. This was neatly resolved with the introduction of Clinitest by Compton and Treneer at Ames in 1945, with a modified copper reagent tablet containing all the reagents required (i.e., sodium hydroxide, citric acid, sodium carbonate and cupric sulphate).[1] |
| The tablet isadded to a small quantity of urine in a tube, which reacts rapidly to generate sufficient heat to cause the mixture to boil. Glucose present in the urine is oxidised, and the blue cupric sulphate reduced, causing a change in colour from blue to green to yellow to orange. Semiquantitative results are obtained by visually comparing the colour formed with a colour chart provided. A similar concept of reagents in tablet form is used to develop a test for measuring ketones in urine in 1950.Nowadays glucose testing strips as shown in Fig.1.are available which give direct results by change of color which is compared to reference chart showing amount of glucose.[1] |
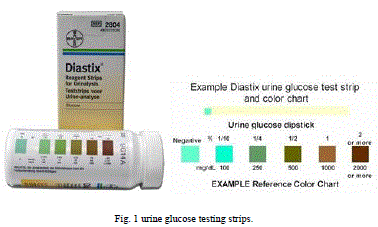 |
Advantages [1] |
| 1. Method is simple. |
| 2. Less expensive. |
| 3. Gives immediate results. |
Disadvantages |
| 1. Non reliable method. |
| 2. Gives less accurate results. |
| 3. A pathologist or qualified person is required to perform the test. |
| 4. The results may vary with change in conditions like temperature, pH...etc. |
| 5. Blood sugar more than renal glucose threshold (180mg/dl) is required to filter out glucose from the kidney and excreted in the urine. |
| 6. Semi-quantitative urine test strips are not as accurate as blood glucose. |
| 7. Reflect increased urine glucose levels a few hours ago, but does not give actual blood glucose level. |
| 8. Neurological disease, prostatitis, renal diabetes and other cases affect the measurement of glucose. |
| 9. urine determination is also affected by many factors: |
| i.Renal insufficiency in the elderly and pregnant patients. |
| ii. Sometimes in non-diabetic patients urine output may increase, such as in certain kidney diseases, a lot of eating, exercise. |
| iii. Urinary tract infection. Women's menstrual period, pregnancy, etc., are not representative of urine glucose. |
| iv.A reduction of some drugs also cause discoloration of urine test strips, resulting in high false urine. Such as vitamin C, salicylates etc. |
From blood analysis |
| Many glucose meters employ the oxidation of glucose to gluconolactone catalyzed by glucose oxidase (sometimes known as GOD). Others use a similar reaction catalysed instead by another enzyme, glucose dehydrogenase (GDH). |
| This has the advantage of sensitivity over glucose oxidase but is more susceptible to interfering reactions with other substances.[2] |
| The first-generation devices as shown in Fig.2.relied on the colorimetric reaction that is still used nowadays in quantitative glucose measurement. Besides glucose oxidase, the test kit contains abenzidine derivative, which is oxidized to a blue polymer by the hydrogen peroxide formed in the oxidation reaction. The disadvantage of this method was that the test strip had to be developed after a precise interval (the blood had to be washed away), and the meter needed to be calibrated frequently. |
 |
| Most glucometers today as shown in Fig.3.use an electrochemical method. Test strips contain a capillary that sucks up a reproducible amount of blood. The glucose in the blood reacts with an enzyme electrode containing glucose oxidase (or dehydrogenase). |
| The enzyme is reoxidized with an excess of a mediator reagant, such as a ferricyanide ion, a ferrocene derivative or osmium bipyridyl complex. The mediator in turn is reoxidised by reaction at the electrode,which generates an electrical current. The total charge passing through the electrode is proportional to the amount of glucose in the blood that has reacted with the enzyme.[3] |
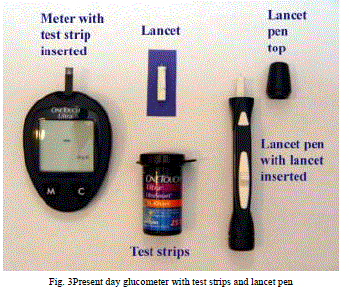 |
Advantages |
| 1. Method is reliable. |
| 2. Method gives high accuracy and precision. |
| 3. Glucometers can be used by patients themselves without any help |
Disadvantages |
| 1. Invasive method so require precautions. |
| 2. Method is costly. |
| 3. The testing strips used in glucometers have short shelf life and show variation in results due to change in operational environmental conditions. |
| 4. Colorimeter used for the analysis requires calibration every time. |
II. RESEARCH & DEVELOPMENT OF NON INVASIVE METHODS |
| Non invasive optical sensors are used frequently in medical field which helps in diagnosis by providing information from blood & tissues as a part of sample. For non-invasive blood glucose measurement various optical methods have been designed & developed. The methods include infrared absorption; near-infrared scattering; Raman, fluorescent, and thermal gradient spectroscopies; as well as polar metric, polarization heterodyning, photonic crystal, optoacoustic, optothermal, and optical coherence tomography (OCT) techniques.[4],[5] |
| ïÃâ÷ Raman spectroscopy is based on the use of a laser light to induce oscillation and rotation in molecules & consequent emission of scattered light influenced by this molecule vibration, which depends on the concentration of the glucose molecule .[6] |
| ïÃâ÷ Infrared spectroscopy is based on absorption and scattering of Infra red light occurs when focused on human tissues due to its interaction with biological components within the tissues. This interaction produces molecular vibration and absorption of energy in infrared region. This vibrational absorption corresponds to the wavelength in order of 4000-400 cm-1. [6] |
| ïÃâ÷ Fluorescent spectroscopy: is based on that when human skin is irradiated with light of specific frequencies it yields fluorescence which can be used for detection of blood glucose.[6] |
| ïÃâ÷ Thermal spectroscopy is based on the concept that human body causes emission of infrared radiation proportionate to glucose absorption. Such absorption is related to glucose concentration.[6],[7] |
| ïÃâ÷ Photo acoustic technology uses the laser for excitation of body fluid & its acoustic response is calculated for blood glucose concentration measurement.[4],[5] |
| ïÃâ÷ The optical coherence tomography (OCT) is based on the use of a low coherence light, such as a super luminescent light, an interferometer with a reference arm and a sample arm, a moving mirror in the reference arm and a photo detector to measure the interferometric signal. Light backscattered from tissues is combined with light returned from the reference arm of the interferometer, and the resulting interferometric signal is detected by the photo detector. [6],[8] |
III. OPHTHALMIC GLUCOSE MONITORING SYSTEM: A NOVEL APPROACH |
Approaches for designing of ophthalmic glucose monitoring system |
1. Amperometric approach |
2. Colorimetric approach |
1. Amperometric approach |
Design and fabrication of a flexible biosensor[9] |
| The glucose sensor has a 3mm x 50mm x 84mm laminar structure as shown in Fig.4., which consists of an enzyme immobilized membrane and film-like oxygen electrode (Pt working electrode and Ag/AgCl reference/counter electrode). The sensor is constructed by immobilizing the enzyme membrane onto the sensitive area of the oxygen electrode. |
| The film-type oxygen electrodes has four layers |
| (i) A flexible gas-permeable membrane (polypropylene, thickness: 25 mm), |
| (ii) A 200 nm thick Pt electrode and a 300 nm thick Ag/AgCl electrode, |
| (iii) A membrane filter with dimensions of 1 mm x 1.5 mm containing electrolytic solution (0.1 mol/l KCl) |
| (iv) A non-permeable membrane (film thickness: 50mm). |
| The wearable glucose sensor is fabricated by immobilizing glucose oxidase onto the sensing region of the flexible oxygen electrode. Glucose oxidase (GOD) is immobilized using water soluble photosensitive resin In order to improve the contact between the gas-permeable membrane and the enzyme immobilized membrane, an aminopropylsilane monolayer is prepared on the surface of the gas-permeable membrane. |
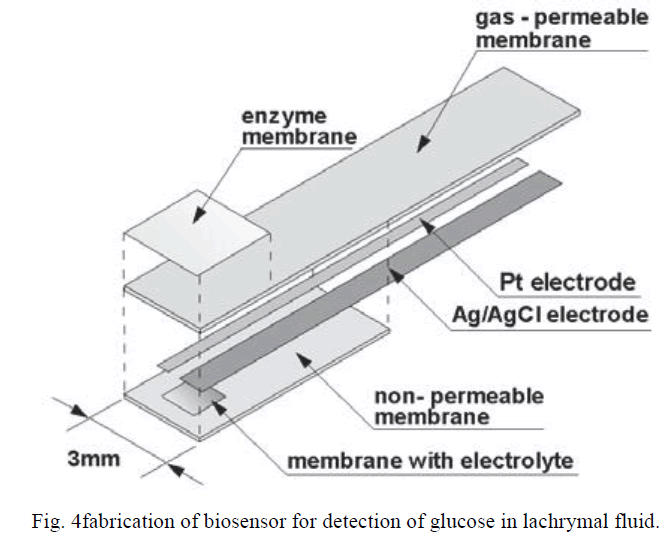 |
| This film strip is fixed to ophthalmic contact lenses which is connected to an chip and antenna which transmits the glucose level to a computer device from the information on the chip as shown in Fig.5. |
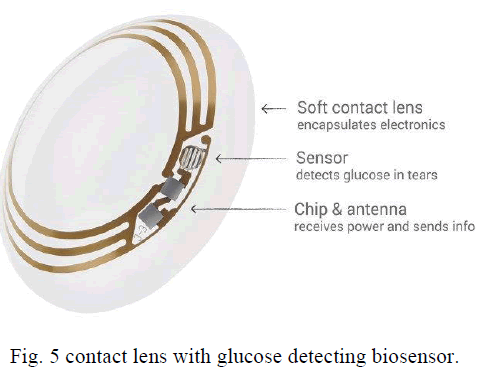 |
Working of the ophthalmic glucose monitoring lens[9] |
| when the lachrymal fluid comes in contact with the sensor embedded on the contact lens the electrode shows the following reactions: |
| Cathode (Pt) : O2+2H2O+4e→ 4OH- |
| Anode(Ag/AgCl) : 4Ag+4Cl →4AgCl+4e- |
| Thus the current generated in the reaction is directly proportional to the amount of glucose present in the lachrymal fluid. |
2.Colorimetric approach |
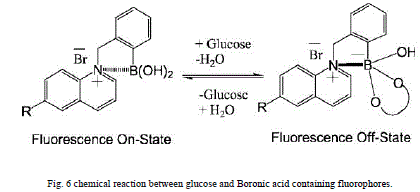
| The sensing material consists of a face-centered cubic array of colloidal particles embedded in a hydrogel (lens) The array spacing is ∼250 nm, designed such that the array diffracts visible light.For glucose sensing boronic acid recognition agents like BAF’s (Boronic acid containing fluorophores) are used which bind to glucose to produce complexes as boronic acid compounds as shown in Fig.6.have high affinity for diol containing compounds such as carbohydrates like glucose.[10] |
Examples of BAF’s [10],[11] |
| 1. BMOQBA: N-(boronobenzyl)-6-methoxyquinolinium bromide |
| 2. BMOQ: N-benzyl-6-methoxyquinolinium bromide. |
| 3. BMQ: N-benzyl-6-methylquinolinium bromide. |
| 4. BMQBA: N-(boronobenzyl)-6-methylquinolinium bromide |
 |
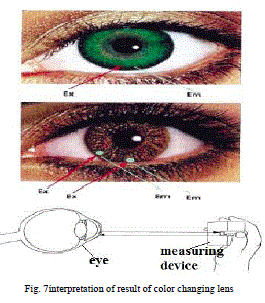 |
| Thus there is change in the color of the lens due to fluorescence caused by complexation of glucose with BAF’s which can be compared to a chart or can be analysed by a device which gives the concentration of glucose in the lachrymal fluid as shown in Fig.7. |
Advantages of the ophthalmic glucose monitoring system[10],[11] |
| 1. It is non-invasive method. |
| 2. It gives quick results. |
| 3. It provides continuous monitoring of blood glucose levels. |
| 4. There is no requirement of withdrawl of biological fluids |
| 5. Suitable for geriatric patients and patients of diabetes having defects of vision as lenses provide correction of vision |
Limitations of the ophthalmic glucose monitoring system[10],[11] |
| 1. Glucose levels in the tears lag 30 minutes behind the blood glucose levels.so exact blood glucose level at a time point cannot be determined. |
| 2. Lenses may produce discomfort to eyes. |
| 3. The lenses are required to be sterilized before and after use. |
| 4. Lenses are expensive. |
| 5. Lenses have a short usage period. |
CONCLUSION |
| The proposed new electrochemical glucose sensing technique using the contact lenses has many potential advantages over currently existing invasive and non-invasive methods. The contact lens glucose sensing method introduced can be miniaturized using current integrated circuit and semiconductor technology, and has the potential to provide a low cost, fast, stable, and compact non-invasive glucose sensor for the diabetic patients within near future. |
References |
|