ISSN ONLINE(2278-8875) PRINT (2320-3765)
ISSN ONLINE(2278-8875) PRINT (2320-3765)
| A.Bonjyotsna1, S.Roy2 Department of Electronics & Communication Engineering, Tezpur University, Tezpur 784028, Assam, India1,2 |
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Advanced Research in Electrical, Electronics and Instrumentation Engineering
This paper reviews the methodology of detecting drowsiness of a person from Electrocardiogram (ECG) signal. ECG is one of the most important physiological biosignal which can be used to study the cardiological behavior of a person. It has become utterly essential nowadays to predict the drowsiness of a person in a situation as important as driving. The Heart Rate Variability (HRV) derived from RR interval time series from the ECG signal plays a significant role for assessment of Autonomic Nervous System (ANS). The HRV signal is subjected to spectral analysis yielding different frequency bands. The low frequency band (LF) and the high frequency band (HF) are the two main parameters which can be used to denote the drowsiness state.
Keywords |
||||||||||
| ECG; QRS detection; RR Interval; Heart Rate Variability (HRV);Frequency Domain Analysis; Power Spectral Density (PSD);. | ||||||||||
INTRODUCTION |
||||||||||
| There are Different Methods for collecting and analyzing physiological data during real-world tasks to determine a person’s relative stress level. The different physiological parameters responsible for determining stress are Electrocardiogram, Electroencephalography, Electromyogram, skin conductance, respiration etc. The results show that for most car drivers studied, skin conductivity and heart rate metrics are most closely correlated with driver stress level. These findings indicate that physiological signals can provide a metric of driver stress in future cars capable of physiological monitoring [1]. Individuals subjected to mental work load exhibit changes in variety of physiological functions. One of the most prominently used signals is the Electro-encephalography (EEG), the electrical activity of the brain [2]. Experiments has been done earlier by different researchers taking different parameters like Electro- Oculogram (EOG), EEG, ECG, Electromyogram (EMG) and skin conductance. It has been established that the variations in the Heart Rate can detect different physical conditions including drowsiness. | ||||||||||
| Since the sleep rhythm is strongly correlated with brain and heart activities, these physiological biosignals can give accurate drowsiness detection. However, all the researches up to date need electrode contacts on drivers’ head, face, or chest. Wiring is another problem for this approach. The electrode contacts and wires will annoy the drivers, and are difficult to be implemented on vehicles. Therefore the heart rate signals are used to detect drowsiness and aims to overcome the limitation of current methods by developing non-intrusive, easily implementable and accurate heart rate sensors [3]. | ||||||||||
| The key to the proposed drowsiness detection approach is to have an accurate and non-invasive heart rate signal measurement system. Other biosignals like EEG or EOG require extra wiring and obtrusive instrumentation which may cause distraction to the driver. | ||||||||||
| Fig. 1 describes the complete process for detecting drowsiness by acquiring only ECG signals. | ||||||||||
REVIEW OF ECG SIGNAL PROCESSING |
||||||||||
| The electrocardiogram (ECG) is a technique of recording bioelectric currents generated by the heart. Clinicians can evaluate the conditions of a patient's heart from the ECG and perform further diagnosis. ECG records are obtained by sampling the bioelectric currents sensed by several electrodes, known as leads from the surface of the body. A typical one-cycle ECG tracing is shown in Fig. 2. | ||||||||||
| Generally, the recorded ECG signal is often contaminated by noise and artifacts that can be within the frequency band of interest and manifest with similar characteristics as the ECG signal itself. In order to extract useful information from the noisy ECG signals, it is required to process the raw ECG signals. | ||||||||||
| ECG signal processing can be roughly divided into two stages by functionality: preprocessing and feature extraction. | ||||||||||
| The preprocessing stage removes or suppresses noise from the raw ECG signal and the feature extraction stage extracts diagnostic information from the ECG signal. Of the many morphological markers of the ECG, the QRS complex and the R-peak are the most significant – with the contribution of the R-peak to the R to R interval being a driving factor. The number of R peaks in a specific time interval translates to the heart rate (in beats per minute) [4]. The instantaneous change in R-R interval (also called Heart Rate Variability or HRV) is of clinical significance | ||||||||||
A. Algorithm for R peak detection |
||||||||||
| Pan and Tompkins [5] have developed an algorithm for ECG R-peak detection. Fig. 3 depicts the important parts of the algorithm. | ||||||||||
| To attenuate noise in this method, the signal is passed through a band pass filter made of cascaded high-pass and lowpass filters. High slopes are found using differentiation, which distinguish the QRS complexes from other ECG waves. | ||||||||||
| Then a nonlinear transformation that involves squaring of the signal samples is done to make the entire data positive before integration. It also highlights the higher frequencies in the signal obtained from the differentiation process. These higher frequencies denote the QRS complex. Then the squared waveform is passed through a moving window integrator and a decision is taken based on threshold detection. The peaks are thus identified from the thresholds. | ||||||||||
REVIEW OF HEART RATE VARIABILITY |
||||||||||
| The interval between adjacent QRS complexes is termed as the normal to normal (NN) or the R to R (RR) intervals. Heart rate variability (HRV) refers to the beat-to-beat alterations in heart rate. Under resting conditions, the ECG of healthy individuals exhibits periodic variation in R-R intervals. The HRV measurements are captured un-obtrusively from the ECG signal. The results from this HRV data are capable of portraying physiological condition of the patient and are an important indicator of cardiac disease. Variability in heart rate is clinically linked to lethal arrhythmias, hypertension, coronary artery disease, congestive heart failure, organ transplant, tachycardia, neuropathy, and diabetes [6]. Heart Rate Variability (HRV) measurements analyse how these RR intervals, which show the variation between consecutive heartbeats, change over time. For example, Fig. 4 shows the HRV of a typical adult. | ||||||||||
A. HRV Analysis Methods |
||||||||||
| There are different methods of HRV analysis. One of the methods is time domain analysis. This method extracts a few special measures using only the temporal RR interval signals. Another method is spectral analysis. This method interpolates the RR interval at a certain rate and transforms this interval into the frequency domain. There are some standards for these two methods [6]. There are also other methods such as Time-Frequency Domain and Nonlinear method. | ||||||||||
1) Frequency Domain Analysis |
||||||||||
| The frequency domain analysis method of HRV analysis extracts frequency domain parameters, such as peak frequency and power in band, from the RR interval signals. The two components of ANS, sympathetic and parasympathetic, increase or decrease the heart rate and influence different bands in the spectrum of RR intervals. Therefore, frequency domain analysis can be used to monitor the state of the ANS. | ||||||||||
| Frequency domain methods usually involve the following three steps: | ||||||||||
| 1. Resample the RR interval signals and linear interpolation. | ||||||||||
| 2. Estimate the power spectral density (PSD) of the RR interval signals by using FFT. | ||||||||||
| 3. Compute frequency domain parameters from the PSD. | ||||||||||
| The HRV is comprised of multiple frequencies. The two main frequency components that represent ANS activity are the low frequency (LF) components (0.04 to 0.15Hz) and the high frequency (HF) components (0.15 to 0.4 Hz). Frequency domain measures confirm that the LF and HF oscillatory components are relative indices of cardiac sympathetic and vagal activity respectively. Normalized units are obtained by the equation[8]. | ||||||||||
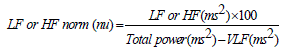 |
||||||||||
| Table I shows the common frequency domain measures of HRV, including peak frequency and power in the very low frequency (VLF), low frequency (LF), and high frequency (HF) bands. | ||||||||||
| The low frequency to high frequency (LF/HF ratio) calculated from power spectrum density (PSD) of subjects’ heart rate time series denotes a person’s drowsiness. The LF/HF ratio shows decreasing trends as subjects go from awake to drowsy. Shan Hu et. al. [3] carried out an HRV analysis during driving simulation in which two health subjects (male, 24 and female, 24) were recruited for two-hour driving simulation. At the beginning, the subjects were not sleepy at all: the eye movements were quick and the body movement was active; whereas at the end, the drivers seemed very sleepy: eye blinking occurred slowly, the eyelids were shut sometimes and yawning happened frequently with deep respiration. The LF/HF ratios for both subjects during driving simulation are shown in Fig. 8. | ||||||||||
| As getting drowsy, both subjects’ LF/HF ratios show a decreasing trend. However, the slope of the trend varies among two subjects. The results of HRV analysis during two-hour driving simulation are in accordance with previous psychophysiological researches on the relationship between sleep stages and HRV [3]. | ||||||||||
| The trend of LF/HF ratio differs for different individuals. There is no conventional range of values for which a person may get drowsy as every individual show different cardiac behaviour. The set of LF/HF values during awake of a subject is considered normal behaviour and a constant decrease in the trend would signify a person’s drowsy state. Fig. 9 depicts the LF/HF trend of three subjects. | ||||||||||
DROWSINESS DETECTION |
||||||||||
| The low frequency to high frequency (LF/HF ratio) calculated from power spectrum density (PSD) of subjects’ heart rate time series denotes a person’s drowsiness. The LF/HF ratio shows decreasing trends as subjects go from awake to drowsy. Shan Hu et. al. [3] carried out an HRV analysis during driving simulation in which two health subjects (male, 24 and female, 24) were recruited for two-hour driving simulation. At the beginning, the subjects were not sleepy at all: the eye movements were quick and the body movement was active; whereas at the end, the drivers seemed very sleepy: eye blinking occurred slowly, the eyelids were shut sometimes and yawning happened frequently with deep respiration. The LF/HF ratios for both subjects during driving simulation are shown in Fig. 8. | ||||||||||
| As getting drowsy, both subjects’ LF/HF ratios show a decreasing trend. However, the slope of the trend varies among two subjects. The results of HRV analysis during two-hour driving simulation are in accordance with previous psychophysiological researches on the relationship between sleep stages and HRV [3]. | ||||||||||
| The trend of LF/HF ratio differs for different individuals. There is no conventional range of values for which a person may get drowsy as every individual show different cardiac behaviour. The set of LF/HF values during awake of a subject is considered normal behaviour and a constant decrease in the trend would signify a person’s drowsy state. Fig. 9 depicts the LF/HF trend of three subjects. | ||||||||||
CONCLUSION |
||||||||||
| The ongoing study and analysis of ECG and its corresponding Heart Rate Variability has led to the prediction of many serious symptoms of cardiac diseases. The analysis of HRV both by time-domain and spectral approaches offer a noninvasive method of evaluating cardiac functioning. The measurement of HRV is becoming increasingly standardized making it convenient to use for medical purposes. In automotive application, the drivers’ physiological signals can be used for research and development of advanced driver active safety applications and assistance systems. | ||||||||||
Tables at a glance |
||||||||||
|
||||||||||
Figures at a glance |
||||||||||
|
||||||||||
|
||||||||||
References |
||||||||||
|