ISSN ONLINE(2278-8875) PRINT (2320-3765)
ISSN ONLINE(2278-8875) PRINT (2320-3765)
Nur Ilham Imarah binti Mou Yusop1, M.B. Malarvili2
|
| Related article at Pubmed, Scholar Google |
Visit for more related articles at International Journal of Advanced Research in Electrical, Electronics and Instrumentation Engineering
Asthma is a common chronic respiratory disease caused by inflammatory in the bronchioles and narrow airways. Tools usually use by doctor to detect signs or symptoms of asthma are spirometer and peak flow meter, and yet there is no tool that is able to monitor the severity of asthma. However, there are obvious drawbacks of the current tools as patients always have bad effect and their symptoms worsen after they performed the maneuvers. Capnography which is used non-invasively to measure the concentration of carbon dioxide in breath out air was recently introduced to overcome the current limitation. This study aims to design a GUI (graphical user interface) to detect the severity of asthma by using MATLAB software. The GUI build will present the data into simpler and friendly program. It consists of patient information part and capnography analysis which is able to detect the severity of asthma. Success of this project widen the usage of capnography in medical areas and the GUI build may serve as new method to help the healthcare professionals to monitor the severity of asthma due to its properties of non-invasive, effort-independent, and continuous monitoring.
Keywords |
| asthma monitoring; capnography; signal processing, GUI; MATLAB; capnogram |
I.INTRODUCTION |
| Asthma is a common chronic respiratory disease which involves the lung. It happened because of the inflammatory in the bronchioles and of airways which make asthmatic patient to have difficulties to breathe in and breathe out. The hallmarks of asthma are the airways and bronchioles become swollen, narrow and extremely sensitive when react to certain inhaled substances. The smaller airways cause air obstruction and regional decreases in airflow which then consequently lead to alveolar ventilation especially during expiration. |
| Asthmatic patient tend to cough, have breath shortness, chest tightness and a wheezing sound can be heard from lungs when the medical doctor listen through auscultation with stethoscope. The factors that trigger asthma can be classified into two groups which are inflammatory trigger or symptom triggers. The inflammatory trigger includes pollens and certain air pollutants while the tobacco smoke and strong chemical fumes like perfume are in symptom triggers group. |
| In Malaysia, asthma is one of common disease treated in the clinics. According to the Third National Health and Morbidity Survey (NHMS III) done in 2006, asthma affect about 10-13% of total population with a large scale of being under-treated and live in poor quality lives. The highest prevalence is among the Malays (67%), followed by Indians (12.9%), other races (10%) and Chinese (7.3%) [1]. Besides that, Asthma Council Malaysia in 2003 revealed that 66% of the asthmatic person never have a lung function test. |
| Traditionally, the hospitals and health clinics in Malaysia are using spirometer and peak flow meter to detect any signs or symptoms of asthma. Peak flow meter will monitor the strength of lung exhalationâÃâ¬ÃŸs by measures the air flow in one “fast blast”. The value recorded is known as peak expiratory flow rate (PEFR) which is used to determine the severity of bronchospasm and the degree of airway obstruction of the patient. By using all this information, the doctors are able to monitor and determine the asthmatic condition. Patient need to take a deep breath as deep as they can and then blow hard as fast as possible and repeat the process about two to three times. However, this method brings some negative feedback to patients as they feel dizzy after use the device. It is a very patient dependent tool and patient must give full cooperation so that the device will be able to detect the clinically important reduction. |
| In other hand, spirometer is an apparatus for measuring the volume of inspired and expired by the lungs. It is use to measure the amount of air a person can hold in its lung and time taken for the lungs to be emptied and filled. Any small changes in lung can be detected by using spirometer before the patient aware of it. Although it is one of useful medical device in management and diagnosis of asthma, it involves big and complex equipments thus it is impossible for patients to buy it and monitor their condition at home by themselves. Besides that, it takes some time to use the device as it requires some training from the clinician or respiratory therapist in order to make sure the test is successfully done. |
| The other method to assess asthma is by clinical assessment. In clinical assessment, the first step done by the doctors is asking about the patientâÃâ¬ÃŸs background and focuses more on the medical history. They want to identify the symptoms, the occurrence and any possible asthma trigger such as allergens. After that, a physical test is conducted especially around the upper respiratory tract. The doctors will listen for wheezing sound and may look for nasal secretion or any similar allergy-related symptoms. The doctor keeps the symptoms record on a diary card and the data obtained is often used in clinical trials. |
| This is the simplest method and takes least time compared to spirometer and peak flow meter, however symptoms may not indicate the severity of disease and there is no strong evidence regarding the patient health. Some physicians may be unsure to determine the degree of airway obstruction [2]. Sometimes, the improvement in airway obstruction is because of oxygen therapy alone. Although the symptoms may be gone after the patients undergo medical treatment, it does not necessarily correlate with patientâÃâ¬ÃŸs health status [3]. |
| Capnography which is non-invasively technique that recently been introduced to monitor asthmatic condition. By using infrared technology, it measures the carbon dioxide ventilation and display a graph called capnogram which consist of instantaneous C02 concentration (mmHg) against time (second). Besides that, the usage of capnography as asthma monitoring tool have been studied years ago and also can be use to assess variety respiratory problems and patients feel more convenient using it compared to spirometer and peak flow meter as patient can comfortably lay and sit down when they use it. |
| In this project, a GUI to monitor the severity of asthma is designed by using MATLAB software. It analyzes features extracted from capnogram signal using reported algorithms in literature review. The GUI is able to classify the patient to asthmatic and non asthmatic group as well as to rate the severity of asthma from scale 1 to 10. The following section elaborates on the overview of capnography and previous study related to capnogram. In section 3, we describe the GUI developed based on the existing study. The results of the GUI and the data analysis are presented in section 4. Lastly, a conclusion is made in section 5. |
II.SYSTEM OVERVIEW |
| Capnography |
| Capnography is a continuous analysis of carbon dioxide (CO2) concentrations in respiratory gases. The graph produced known as capnogram displays plot of exhaled carbon dioxide levels (mmHg) over time. The capnogram can be shown either in digitally display (by using machine) or manually measurement (in paper tracing). |
| Capnometry is the measurement and numerical display of maximum level during respiratory cycle. It was first used during the Second World War to monitor the submarines internal environment [4]. It then was used experimentally in 1950s to measure the expired CO2 during anaesthesia procedure and it was used widely in 1980s mainly in anaesthesia practice [5]. Right now, capnography had been used not only in realms of anaesthesia, but also use to monitor patients with impaired respiratory function and to detect changes in respiratory tract. |
| A normal capnogram shapes slightly like square wave pattern as shown in Figure 1. Expiratory consist of three successive phases: (1) a latency phase (Phase I), corresponding to the expiration of the anatomical dead space (PexpCO2 = 0), which is indistinguishable from the preceding inspiration; (2) slope phase (Phase II) marked by a very rapid rise in (PexpCO2), corresponding to the expiration of mixed air; and (3) plateau phase (Phase III), reflecting the elimination of alveolar air (slightly increasing PexpCO2), resulting in the peak at the end of tidal expiration (PetCO2 close to alveolar carbon dioxide tensions) [6, 7]. The highest peak in the capnogram is known as the end-tidal point |
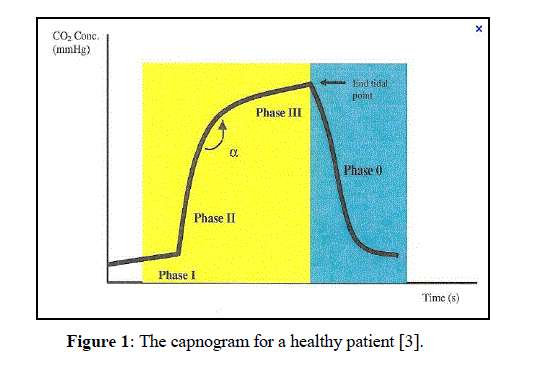 |
| For an asthmatic patient, the airways are swollen, narrow and have extra mucus plugging which cause regional decrease in airflow and alveolar ventilation. The desynchronization in capnogram shape happened when the carbon dioxide is released at different times during expiration. The mixed of alveolar air from bronchioles region with dead space in the lung deformed the capnogram shape. Phases II losses its verticality, alpha angle (which also known as angle Q) between Phase II and Phase III is widely opened and Phase III have increased inclination [6]. In severe asthmatic state, the capnogram comes out like a „shark finâÃâ¬ÃŸ as shown in Figure 2. The researchers are interested with the capnogram changes as it indicates changes in respiratory system. |
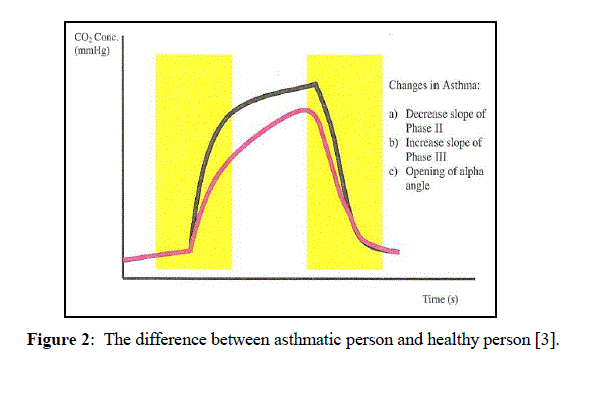 |
| Previous study related to capnography |
| The B.You et al. [5] studied the asthmatic capnogram manually. The parameters suggested were S1, S2, S3, SR to analyze the capnogram. The initial slope from 0 to 0.2 seconds is the S1 region while S2 measures the middle slope from 0.8 to 1.2 seconds. SR is the slope ratio between S1 and S2 [SR = (S2/S1) x 100]; A1 calculated as the area under the curve at 0.2 to 1 seconds while A2 is the rectangle area. AR is the ratio calculated from [(A1/A2) x 100]. B.You did an experiment to measure the capnographic measurements of the 40 subjects (10 asthmatic and 30 control subjects) and compared the result to the spirometric indices. He found that there was significant correlation (p<0.001) between spirometry and capnography indices but the strongest were at the intermediate phase and the angle between E2 and E3, hence capnography is able to used in study of asthmatic patient condition. |
| In 1995, Yaron M. did a similar concept experiment with B.You but he was using peak flow meter [8]. In his experiment, the end-tidal of C02 waveform from 20 asthmatic subjects and 28 normal adult were recorded and the best of three peak expiratory flow rate was recorded. The dCO2/dt values and the correlations between the data were calculated. In the study, they found that the dCO2/dt was interrelated with the PEFR (r = 0.84, p<0.001) and dCO2/dt of the alveolar plateau can be used to detect bronchospasm. |
| CV Eagleston [9] in 1997 examined the possibility of using capnography as an airway obstruction indicator in nonintubated room patient. By using a nasal capnogram cannula, 38 admitted patients were checked for the presence of expiratory wheeze. The capnogram traces were analyzed and the slope ratio was obtained. As the result, he found that there was significance difference in the mean value for SR between the two groups (p<<0.001). The mean value for SR of patient with normal morphology was 7.57 (SEM 0.18) with 95 CI 6.37 to 8.77 while the mean value for SR of patient with obstructive evidence was 31.9. The capnogram of asthmatic person also showed obstructive “sharkâÃâ¬ÃŸs fin” morphology. He also concluded that the capnography may be to monitor respiratory condition continuously in order to find the airway obstruction in acutely ill patients. |
| An experiment to determine if bronchospasm changes in acute non-intubated asthmatic patients are related to changes in the Phase 2, Phase 3 as well as the alpha angle opening in capnogram can be a was carried out by TeoAik Howe in 2008 [3]. 30 acute asthmatic patients were monitored with clinical severity score and peak flow measurements. The patients also had a nasal cannula sampling. A second set of capnographic waveform was recorded if the patients improved enough after treatment for discharge. The results before treatment and after treatment were tested by using t - test analysis. |
| There was a significance result for phase III (p<0.001) and alpha angle (p<0.001) on the capnographic waveform of the pre-treatment and the post-treatment, but phase II showed different outcomes (p<0.35). Hence, they concluded that there were significance changes in peak flow meter reading but it was weakly correlated with the capnographic indices. The study also provides some early findings showing that the capnographic waveform indices can show improvement in the airway diameter in acute asthmatics. |
| A new algorithm to rate the severity of asthma was created by Mohsen Kazemi and MB Malarvili [10] in 2012. By using new processing techniques, he combined the linear predictive coding (LPC) coefficients and autoregressive (AR) modeling techniques to process the capnogram signals. After tested the effectiveness of extracted features by using ROC technique, the algorithms built by him now was able differentiate asthmatic and non-asthmatic patients. It also able to detect the severity of asthma with rating scale 1 to 10 and comes out with an high detection rate of 95.64% and small error rate of 4.34%. |
| From the information collected based on the previous studies, we can conclude that the capnography signal contain special features that reflect changes in respiratory system. By using suitable algorithm, the features extracted are gathered to produce a GUI that can monitor the severity of asthma. |
III. METHOD |
| This section discusses on the steps done in order to build a GUI that is able to monitor the severity of asthma. This research method started with gathering relevant and detailed literature review on the capnography. Then, the GUI layout was designed first before implementation process by using MATLAB software. Last step was GUI optimization by adding up patient information and patient medical background parts. The overall processes done in this project is simplified into a flow chart shown below in Figure 3. |
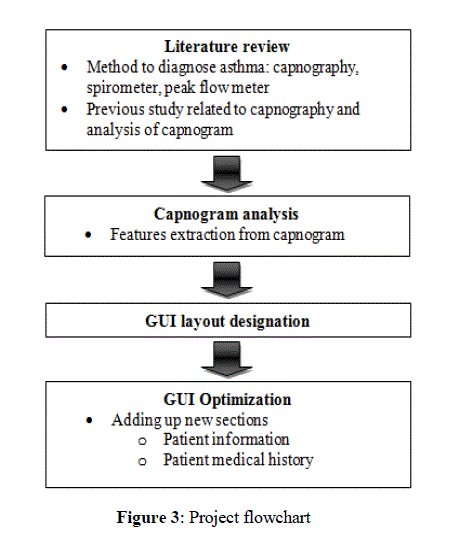 |
| GUI implementation |
| Graphical user interface or GUI (pronounced as goo-ee) allows the user to interact with programs more friendly and easy to use. The method behind the GUI is “what you see is what you get”. The user does not have to memorize complicated command language and type them in order to get the result. GUI allows the user to perform the analysis of capnogram signal easier rather than typing MATLAB coding in the command window. GUI for capnogram signal analysis was created using functions available in the Matlab. |
| The flow of GUI for this project that has been implemented in this project can be illustrated into a flowchart as shown in Figure 4 below. |
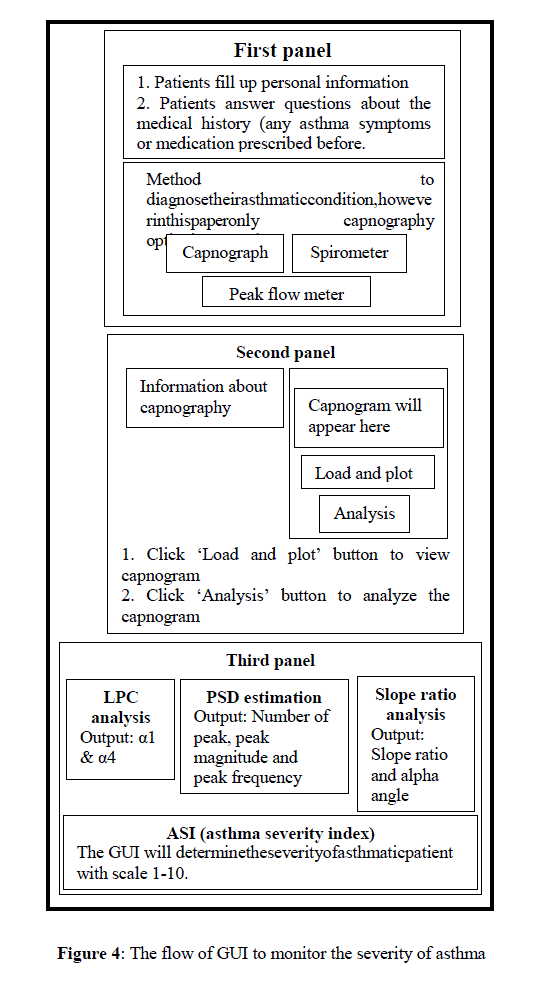 |
IV. RESULT AND DISCUSSION |
Graphical user Interface (GUI) |
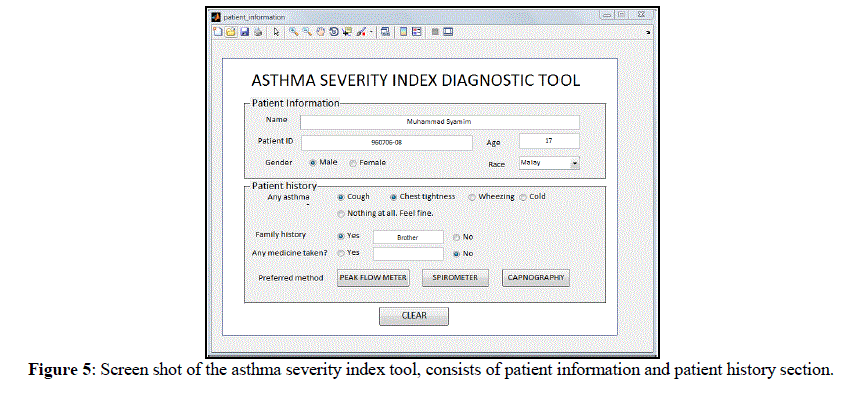
| Figure 5 shows the GUI screen shot. It consists of two sections, patient information and history section. Patient can fill up their details and answer the related medical questions. The questions prepared in the GUI are the frequently asked questions by the doctors to patients.Afterthat, patient able to choosetheirpreferred methodto diagnosetheirasthmaticcondition,howeverinthisprojectonly capnography optionis presented. |
| The patient information and medical history section are vital part in patient assessment and remain as the first thing done during clinical practice. Besides that, it is said that over 80% of diagnoses are made on history alone, a further 5- 10% on examination and the remainder is on investigation [11]. A number of information are collected in comprehensive patient histories, including presenting conditions, past medical history, family history, medication use and their social status. The information collected will provide the doctor some ideas about the health condition of their patient [2]. |
 |
| ThesecondsectionoftheGUIisdesigned to analyze the capnogram signal. It gives parameters such as width ofalphaangle,gradientofsloperatioas wellas theLPC coefficients andPSDestimation.Thecombinationofthe featuresisable todeterminetheseverityofasthmaticpatient. Figure 6 shows example of capnogram analysis for a non-asthmatic patient. |
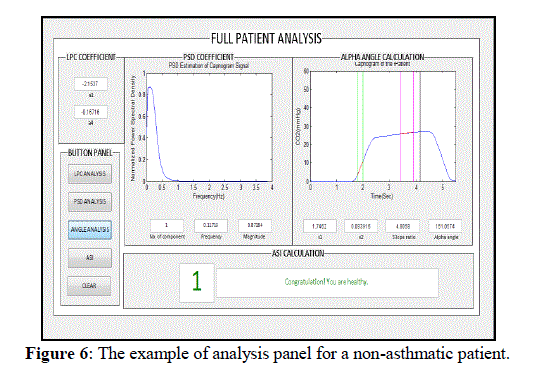 |
| The GUI comes out with LPC analysis, PSD estimation, slope ratio analysis and asthma severity index. A healthy patient is rated with scale 1, scale 2-6 for severe asthmatic while scale 7-10 indicates that the patient has serious asthma. |
| Data analysis |
| The capnogram signals were processed by using signal processing techniques; which were LPC analysis and AR modeling techniques. Then, the methods used by previous researcher to analyzecapnogram such as alpha angle and slope ratio analysis were combined in order to increase the efficiency of asthma diagnostic tool. |
1) LPC Analysis |
| LPC is a method used in source of signal modeling through the observation of input and output sample sequences [10] LPC analysis functions by estimation of a functional set of component coefficients which describe the behavior of as system where each expression is approximated as a combination of past samples [13]. LPC analysis will guess the best estimation coefficient over the number of sample data and produce a good approximation of the original expression sample [14]. By using LPC analysis, there are two parameters that are extracted which are α1 and α4. More info on the suitability of LPC and the results can be found at [10] |
2) AR Modelling |
| Autoregressive (AR) models are generally used for power spectral density estimation [15]. It is mainly used to estimate the power spectral density of biomedical signals [10]. In order to obtain the power spectrum, the time domain capnogram signal will be converted into frequency domain by using fast Fourier technique (FFT). From the spectrum, there are two important parameters to extract for further analysis of capnogram signal. They are number of peak maximum or dominant spectral PSD as well as the frequency and magnitude of at the PSD. |
3) Alpha angle and slope ratio analysis |
| The alpha angle and slope ratio analysis proposed by B. You et al (1994) was included to increase the effectiveness of the tool. The parameters are S1, S2, SR and alpha angle calculation. The first inflection where the capnogram takes a steep rise during early respiration was identified to be the curves rises above a CO2 partial pressure of 4mmHg [3]. The next obvious inflection point was identified as the end tidal peak, where the sharp drop of CO2 partial pressure curve is happen here. With that in considerations, S1 was calculated as the gradient of the curve formed from the point where capnogram rises above 4mmHg, for duration of 0.25 seconds. At this level, the CO2 has to have come out from lungs to reach a level of 4mmHg. S2 was the gradient of the curve at 0.75 seconds to 0.25 seconds from the end tidal peak [3]. Slope ratio was calculated from (S2/S1) x 100. α angle was the intersection angle between slope of S1 and slope of S2 [5]. |
| Until now, there is no asthma severity monitoring tool yet. The various options available to assess airway obstruction which are clinical assessment, peak flow meter estimation and by using spirometer have their own disadvantages. Hence, capnography which is an ideal respiratory monitoring that would not rely heavily on patient compliance or require the interruption of any medication while giving a real time graphic display has been introduced to overcome this problem. Although the studies between capnography analysis and the correlation with bronchospasm had been done years ago, most of the experiments were conducted in conventional time-domain methods with assumptions that the capnogram is a stationary signal [10]. |
| B.You et al studied about the relationship between peak flow meter and the end tidal slope which was manually measured and they were among the first to suggest the usefulness of computerization of capnogram analysis [3, 5]. This is due to the difficulty to identify constant or specifics within each waveform for repeatable and reproducible analysis [16].The development of computerized methods which can recognized the different waveform morphologies could benefit both healthcare professional involved in respiratory care and the patients. This method also could further assist the doctors and medical staff to monitor severity of asthma automatically and instantaneously. |
V.CONCLUSION |
| Monitoring asthma by using capnography is a new approach in medical technology and it is not yet widely used in Malaysia. As the current method to monitor and manage the presence of asthma posses limitation, monitoring by using capnography is an alternative way to solve the limitations. In this project, a GUI to detect and monitor the severity of asthma was successfully created by using existed algorithms, capnogram features extraction and combined the features found by the previous researcher to enhance the efficiency of the tool. Computerize analysis of capnographic waveform may extend the usage of capnography in medical areas and promote the use of capnography for the purpose of monitoring asthmatic patient during asthmatic attack. With further research, capnography may serve as a new method in monitoring asthma as it has great potential due to its properties of non-invasive, effort-independent, and continuous monitoring. Also, in future, analysis of asthmatic patient using the peak flow meter and spirometer will be included in the GUI so that a complete monitoring tool can be produced to monitor severity of asthma. |
References |
|