Our goal is design a Non- Invasive Patient monitoring system and to provide the information about calculation of insulin units provide for the particular patient by the system itself. Wireless, patient monitoring system and control using and GSM technology is used to monitor the different parameters of an ICU patient remotely and also control over medicine dosage is provided. Measurement of vital parameters can be done remotely and under risk developing situation can be conveyed to the physician with alarm triggering systems in order to initiate the proper control actions. In the implemented system a reliable and efficient real time remote patient monitoring system that can play a vital role in providing better patient care is developed. This system enables expert doctors to monitor vital parameters viz body temperature, blood pressure and heart rate of patients in remote areas of hospital as well as he can monitor the patient when he is out of the premises. The system in addition also provides a feedback to control the dosage of medicine to the patient as guided by the doctor remotely, in response to the health condition message received by the doctor. Mobile phones transfer measured parameters via SMS to clinicians for further analysis or diagnosis. The timely manner of conveying the real time monitored parameter to the doctor and control action taken by him is given high priority which is very much needed and which is the uniqueness of the developed system. The system even facilitates the doctor to monitor thepatient's previous history from the data in memory inbuilt in the monitoring device. Also data can be sent to several doctors in casea doctor fails to respond urgently. Keywords- Wireless, Remote patient monitoring, Body temperature, Heart rate, Blood pressure, SMS, GSM, ICU.
Keywords |
| Diabetic Mellitus Glucose sensor; Non-invasive; Hyperglycemia hypoglycemia micro controller |
INTRODUCTION |
| The project tells about the Human glucose level monitoring system in wireless mode. Our goal is to design a
finger based monitoring system which is used to measure the patient without blood loss, and calculate the
insulin level to inject patient and send the data through wireless mode.In the implemented system a reliable and
efficient real time remote patient monitoring system that can play a vital role in providing better patient care is
developed. This system enables expert doctors to monitor vital parameters viz body temperature and heart rate
of patients in remote areas of hospital as well as he can monitor the patient when he is out of the premises. The
system in addition also provides a feedback to control the dosage of medicine to the patient as guided by the
doctor remotely, in response to the health condition message received by the doctor. Mobile phones transfer
measured parameters via SMS to clinicians for further analysis or diagnosis. The timely manner of conveying
the real time monitored parameter to the doctor and control action taken by him is given high priority which is
very much needed and which is the uniqueness of the developed system.non- invasive way to detect blood sugar
level.The system even facilitates the doctor to monitor the patient's previous history from the data in memory
inbuilt in the monitoring device. Also data can be sent to several doctors in case a doctor fails to respond
urgently |
GLUCOSE MEASUREMENT |
| Glucose can be measured in whole blood or serum (ie, plasma). Historically, blood glucose values were given in
terms of whole blood, but most laboratories now measure and report the serum glucose levels. Because red
blood cells (erythrocytes) have a higher concentration of protein (eg, hemoglobin) than serum, serum has a
higher water content and consequently more dissolved glucose than does whole blood. To convert from wholeblood
glucose, multiplication by 1.15 has been shown to generally give the serum/plasma level.[1]Collection of
blood in clot tubes for serum chemistry analysis permits the metabolism of glucose in the sample by blood cells
until separated by centrifugation. Red blood cells, for instance, do not require insulin to intake glucose from the
blood. Higher than normal amounts of white or red blood cell counts can lead to excessive glycolysis in the
sample with substantial reduction of glucose level if the sample is not processed quickly. Ambient temperature
at which the blood sample is kept prior to centrifuging and separation of plasma/serum also affects glucose
levels. At refrigerator temperatures, glucose remains relatively stable for several hours in a blood sample. At
room temperature (25 °C), a loss of 1 to 2% of total glucose per hour should be expected in whole blood
samples. Loss of glucose under these conditions can be prevented by using Fluoride tubes (ie, gray-top) since
fluoride inhibits glycolysis. However, these should only be used when blood will be transported from one
hospital laboratory to another for glucose measurement. Red-top serum separator tubes also preserve glucose in
samples after being centrifuged isolating the serum from cells. |
| Particular care should be given to drawing blood samples from the arm opposite the one in which an intravenous
line is inserted, to prevent contamination of the sample with intravenous fluids. Alternatively, blood can be
drawn from the same arm with an IV line after the IV has been turned off for at least 5 minutes, and the arm
elevated to drain infused fluids away from the vein. Inattention can lead to large errors, since as little as 10%
contamination with 5% dextrose (D5W) will elevate glucose in a sample by 500 mg/dl or more. Remember that
the actual concentration of glucose in blood is very low, even in the hyperglycemic.[3] |
| Arterial, capillary and venous blood have comparable glucose levels in a fasting individual. After meals venous
levels are somewhat lower than capillary or arterial blood; a common estimate is about 10%.[7] |
MEASUREMENT TECHNIQUES |
| Two major methods have been used to measure glucose. The first, still in use in some places, is a chemical
method exploiting the ''nonspecific reducing'' property of glucose in a reaction with an indicator substance that
changes color when reduced. Since other blood compounds also have reducing properties (e.g., urea, which can
be abnormally high in uremic patients), this technique can produce erroneous readings in some situations (5 to
15 mg/dl has been reported). The more recent technique, using enzymes specific to glucose, are less susceptible
to this kind of error. The two most common employed enzymes are glucose oxidase and hexokinase. |
| In either case, the chemical system is commonly contained on a test strip, to which a blood sample is applied,
and which is then inserted into the meter for reading.[4] Test strip shapes and their exact chemical composition
vary between meter systems and cannot be interchanged. Formerly, some test strips were read (after timing and
wiping away the blood sample) by visual comparison against a color chart printed on the vial label. Strips of this
type are still used for urine glucose readings, but for blood glucose levels they are obsolete. Their error rates
were, in any case, much higher. |
| Urine glucose readings, however taken, are much less useful. In properly functioning kidneys, glucose does not
appear in urine until the renal threshold for glucose has been exceeded. This is substantially above any normal
glucose level, and so is evidence of an existing severe hyperglycemic condition. However, urine is stored in the
bladder and so any glucose in it might have been produced at any time since the last time the bladder was emptied. Since metabolic conditions change rapidly, as a result of any of several factors, this is delayed news
and gives no warning of a developing condition. Blood glucose monitoring is far preferable, both clinically and
for home monitoring by patients. |
BLOCK DIAGRAM |
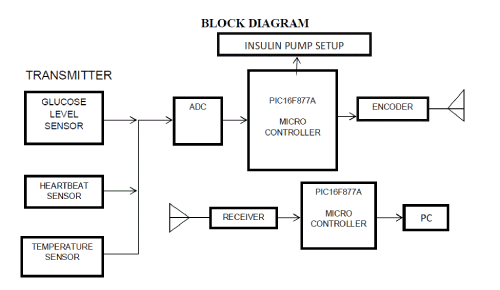 |
WORKING PRINCIPLE |
| This project involves a simple principle of displaying the sensed signal from the sensors on the LCD Screen
through a microcontroller. The sensed signal will be in milli voltage, so it can’t be used directly by the other
components. So the signal is amplified to an extent that can be processed by other components. The amplified
signal is conditioned for the microcontroller by the signal conditioner. The microcontroller, the signal
conditioner and other components are powered by a separate power supply circuit which converts 230V AC to
5V & 12V. The microcontroller is programmed to convert the input signal in volts to the respective glucose
value. The computed value is then displayed in the 16x2 LCD screen |
HEARTBEAT SENSOR |
| A custom heart beat sensor was designed to read the patient’s beats per minute (bpm). The designed sensor is
very small and inexpensive. The technique used to measure the heart rate is based on near-infrared spectroscopy
(NIR). NIR involves using light in the wavelength of 700–900 nm to measure blood volume. At these
wavelengths most tissues do not absorb light – other than haemoglobin This allowed for designing a noninvasive
and low cost method of measuring the pulse. A silicon phototransistor, moulded into a flat side-facing
package, and a GaAs Infrared Emitting Diode were used in the sensor. The amount of light that was detected by
the phototransistor varied with the patient’s heart pulse, as the amount of absorbed |
| IR light changed with the flow of blood, which is directly linked to the heart rate. This signal was then
amplified, filtered, and sent to the microcontroller to be analyzed. The heart rat |
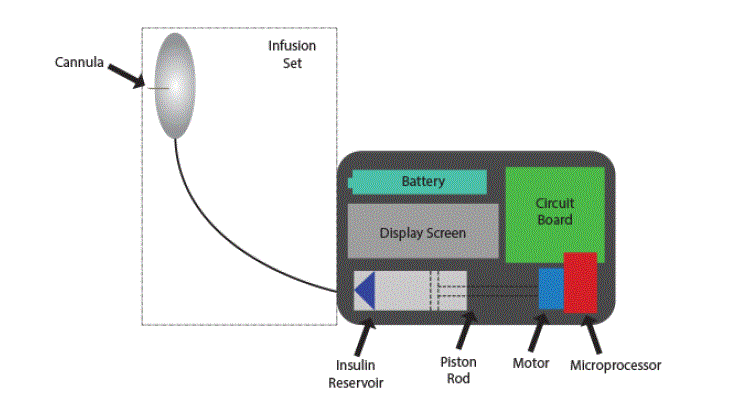
INSULIN PUMP SETUP |
| Insulin pumps provide a precisely controlled rate of insulin delivery to diabetic patients who would normally
need multiple daily injections to regulate blood glucose levels. Insulin pumps improve patient quality of life and
reduce the incidence of long-term complications by providing tighter control of blood glucose levels. The
firmware allows numerous modifications to the bolus dose and basal rate to enable patients to manage insulin
levels in response to (and in anticipation of) events such as eating, sleeping, and exercise. The insulin is
contained in a user-replaceable cartridge held inside the pump. This reservoir is effectively a specialized syringe
with a piston that is slowly pressed by the pump. The cartridge output is connected to flexible tubing going to
the patient’s subcutaneous injection site, usually on the abdomen. A related product for managing diabetes is a
continuous blood glucose monitor. This device provides real-time glucose-level monitoring through a
subcutaneous sensor. The sensor can be left in place for several days at a time, which reduces the need for the
patient to test multiple individual blood samples. Future developments are expected to close the loop between
these two systems by continuously monitoring the glucose level and, in response, automatically adjusting insulin
dosage levels. |
PUMPING AND SENSING APPROACHES |
| Insulin is measured in “units” where there are 100 units per cc (or mL), assuming the standard U-100
concentration. This means that one unit is 10μL. Basal rates are on the order of one unit/hour administered every
three to ten minutes, while bolus doses are several units. Typical cartridge volumes are 200 to 300 units |
 |
TEMPERATURE SENSOR |
| The skin temperature measurement is done using an integrated circuit, the temperature sensor produced by
MAXIM – Dallas Semiconductor . The Sensor gives an analog output depending on the measured temperature.
This voltage has to be measured by the microcontroller using a 12 bit Analog-to-Digital converter (ADC)., used
as temperature sensor This sensor is mounted within the wrist strap, positioned in such a way that it is in
contact with the skin, allowing it to measure the external temperature of the skin. From the skin temperature, the
body temperature is estimated. There can be different methods to estimate the exact body temperature from skin
temperature, but with a rough estimation usually the body temperature is 5.1 C higher than skin temperature
when the body temperature is measured at the ear by the National DM-T2-A thermometer used by a general
practitioner compared to the skin temperature measured at the wrist. Because an exact measurement of body
temperature is not required, this method is suitable. Rather, relative changes are monitored within set threshold,
which sets off the alarm. This allows the device to detect changes in body temperature that could indicate the
patient is undergoing any of the following conditions: trauma, injury, heart attack, stroke, heat exhaustion, and burns. The Output of the
ADC has to be converted into the right value. The ADC-value is first compared with the Reference Voltage of
2.4 V (1) and then with the characteristic of the DS 600 to get the Value for the Temperature. |
CONCLUSION |
| This paper presented an approach to non-invasive blood parameter determined. The Blood glucose monitoring
system accurately measures blood glucose levels over a wide range of glucose values. |
References |
- A. S. Fauci, E. Braunwald, D. L. Kasper, S. L. Hauser, D. L. Longo, J. L. Jameson, and J. Loscalzo, Harrison’s Principles of Internal Medicine, 17th Edition, 17th ed. McGraw-Hill Professional, 3 2008.
- A. Petrie and C. Sabin, Medical Statistics at a Glance, 3rd ed. Wiley Blackwell, 8 2009.
- M. U. M. Update, HandbuchDiabetologie (Handbuch Update-Seminar) (German Edition), 1st ed. Springer, 3 2010.
- K. Doerner, H.-J.Battista, F. Bidlingmaier, and T. Deufel, KlinischeChemie und Haematologie.Thieme, Stuttgart, 9 2001.
- P. J. W. Debye, Polar molecules. Dover Publications, 1960.
- A. Knocks, “Dielektrischespektroskopie an lsungenkleiner, biochemischrelevantermodellsysteme,” Ph.D. dissertation, Ruhr-University Bochum, 2001.
- R. W. L. S. Gabriel and C. Gabriel, “The dielectric properties of biological tissues: Iii. Parametric models for the dielectric spectrum of tissues,” Phys. Med. Biol., vol. 25, no. 6, p. 1149, 1996.
- D. Deslandes and K. Wu, “Integrated micro strip and rectangular waveguide in planar form,” Microwave and Wireless ComponentsLetters, IEEE, vol. 11, no. 2, pp. 68 –70, Feb. 2001.
|